About ketamine therapy

Experience clarity, relief, and meaningful change
If you are still struggling and other treatments haven’t given you the results you hoped for, ketamine therapy may offer a new direction. By enhancing neuroplasticity, your brain can create new pathways for healing.
Starting at $750
Take the first step toward healing → Call our office to see if you’re a candidate

Experience clarity, relief, and meaningful change
If you are still struggling and other treatments haven’t given you the results you hoped for, ketamine therapy may offer a new direction. By enhancing neuroplasticity, your brain can create new pathways for healing.
Starting at $750
Take the first step toward healing → Call our office to see if you’re a candidate
Advanced Ketamine Therapy for Pain & Mood Relief
At Prime Youth Aesthetics, we combine medical expertise and modern science to offer ketamine infusions that help ease chronic pain, relieve symptoms of mood disorders, and activate the body’s innate healing potential.
How Ketamine Can Be Used
Ketamine for Mood Disorders
Ketamine therapy is a fast-acting treatment for mood disorders, including treatment-resistant depression and bipolar depression. It works by targeting glutamate pathways in the brain, helping improve mood and reduce symptoms when traditional medications have not been effective.
-
Ketamine Therapy for Major Depression
In recent years, medical research has shown that low-dose ketamine can relieve depressive symptoms rapidly, often within hours especially in people who have not improved with standard
antidepressants.
There are two main clinical forms used in depression care:
- Intravenous (IV) ketamine given in a monitored medical setting
- Esketamine nasal spray (Spravato) a ketamine-derived medication FDA-approved for treatment-resistant depression and depressive symptoms with suicidal thoughts when administered in a certified clinic.
How Ketamine Works
Unlike traditional antidepressants that target serotonin or norepinephrine, ketamine works on the glutamate system in the brain, a different neurotransmitter pathway linked with mood and neural connectivity. This unique mechanism is thought to rapidly enhance neural signaling and plasticity, leading to quicker mood improvement.
Why Patients Consider Ketamine
Ketamine may be offered when:
- Other antidepressants (SSRIs, SNRIs, etc.) haven’t worked
- Symptoms are severe or include suicidal thoughts
- Rapid relief is important for safety or quality of life
Some studies show that ketamine therapy can reduce depressive symptoms more quickly than traditional treatments, sometimes within hours and improve response rates in treatment-resistant depression.
What the Research Shows
Scientific evidence from hundreds of randomized trials and systematic reviews supports that:
- Ketamine can produce rapid antidepressant effects in major depression.
- Repeated treatments may help sustain mood improvement beyond the first dose.
- Effects tend to start quickly, but like all therapies, they vary by individual.
What to Expect in Treatment
- Before treatment: Your care team will review your medical history, current medications, and mental health symptoms to determine if ketamine is appropriate.
- During treatment: Ketamine is given medically at low doses that do not induce sedation like anesthesia. You’ll be monitored for vital signs and comfort throughout.
After treatment: Some people notice improvement within hours, while others need a series of sessions for best results. Response varies- ketamine is a treatment, not a cure. Continued therapy and medical follow-up are important.
Risks & Side Effects
Ketamine is generally safe when administered in a clinical setting but it is not without side effects. Most are temporary and resolve soon after treatment.
Common effects may include:
- Dissociation or feeling “detached”
- Elevated blood pressure
- Dizziness or nausea
- Mild anxiety or restlessness
Because ketamine affects perception and blood pressure, treatments are not done at home and require medical supervision. Long-term safety data are still emerging, especially with repeated courses.
Important Things to Know
- Ketamine (the standard anesthetic drug) itself is not FDA-approved for depression but esketamine (Spravato) is approved for treatment-resistant depression under supervision.
- Not everyone responds to ketamine, and multiple sessions may be needed.
- Ketamine should only be offered in a controlled clinical environment with monitoring.
Where to Learn More
Here are some peer-reviewed and trusted sources you can reference or link for patients who want to dig deeper:
- PubMed systematic review on ketamine’s antidepressant effects: https://pubmed.ncbi.nlm.nih.gov/37593223/
- Meta-analysis of IV ketamine and depressive symptom reduction: https://pmc.ncbi.nlm.nih.gov/articles/PMC10430179/
- Ketamine vs ECT study (Mass General Brigham): https://www.massgeneralbrigham.org/en/about/newsroom/press-releases/study-finds-ketamine-effective-as-ect-for-major-depression
-
Ketamine for Obsessive-Compulsive Disorder (OCD)
Medical Understanding
OCD is linked to abnormalities in brain circuitry involving glutamate, serotonin, and cortico-striatal-thalamic loops. Traditional first-line treatments include:
- SSRIs
- Cognitive Behavioral Therapy (CBT) with Exposure and Response Prevention (ERP)
However, many patients do not respond fully to these therapies.
How Ketamine May Help
Studies suggest that ketamine may produce rapid reductions in obsessive and compulsive symptoms, often within hours to days after infusion, though effects are typically short-lived (days to weeks) without additional therapy.
Mechanisms proposed include:
- modulation of glutamate neurotransmission
- increases in GABA activity in key brain regions
- enhanced neuroplasticity
Ketamine may also enhance engagement with therapy like CBT/ERP when used alongside it.
What the Evidence Shows
A meta-analysis of ketamine studies found significant reductions in OCD severity on standardized scales like the Y-BOCS after treatment. https://pubmed.ncbi.nlm.nih.gov/39564613/
-
Ketamine Therapy for Post-Traumatic Stress Disorder (PTSD)
Medical Understanding PTSD involves persistent re-experiencing of traumatic events, avoidance, hyperarousal, and changes in mood and cognition. Glutamate dysfunction, stress-related neurocircuitry alterations, and impaired synaptic connectivity are implicated in chronic PTSD.
How Ketamine May Help
Ketamine’s rapid effects on glutamate, synaptic plasticity, and neurocircuitry may help:
- reduce intrusive memories
- disrupt over-consolidated traumatic fear responses
- improve mood and reduce associated depression and avoidance
These effects may be most pronounced shortly after treatment and can be enhanced when paired with trauma-focused psychotherapy.
What the Evidence Shows
- Randomized trials show that single doses of ketamine can significantly reduce PTSD symptom severity compared with placebo or controls at 24 hours. https://jamanetwork.com/journals/jamapsychiatry/fullarticle/1860851
- Systematic reviews and meta-analyses report that ketamine treatment is associated with significant reductions in PTSD symptom scores on measures like PCL-5 and CAPS-5. https://www.cambridge.org/core/journals/cns-spectrums/article/abs/ketamine-for-the-treatment-of-psychiatric-disorders-a-systematic-review-and-metaanalysis/6A857E9466AE391F5A3FE140FDD9F37A
- Combined ketamine + therapy protocols show preliminary evidence of durable improvement in treatment-resistant PTSD. https://pubmed.ncbi.nlm.nih.gov/39199113/
-
Ketamine Therapy for Anxiety Disorders (General Anxiety • Social Anxiety • Panic
Medical Understanding
Anxiety disorders: including generalized anxiety, social anxiety, and panic, involve dysregulation in fear circuitry, neurotransmitters like GABA and glutamate, and hyper-reactivity in stress pathways.
How Ketamine May Help
- By modulating glutamate and enhancing neural plasticity, ketamine may:
- temporarily reduce excessive anxiety signaling
- interrupt entrenched anxiety responses
- improve access to therapeutic engagement
What the Evidence Shows
A systematic review and meta-analysis of randomized controlled trials found that acute ketamine significantly improved anxiety ratings in several anxiety-related conditions, including generalized and social anxiety, and PTSD under anxiety measures. https://pubmed.ncbi.nlm.nih.gov/34925757/
Evidence is preliminary, and optimal dosing and maintenance protocols are still under investigation, but early findings support ketamine’s role as an anxiolytic treatment especially in treatment-resistant cases.
-
Ketamine for bipolar depression
Bipolar disorder includes mood swings from depression to mania/hypomania, and depressive episodes are often the most disabling and hardest to treat. Traditional antidepressants have limited effectiveness in bipolar depression and can sometimes trigger mania — which is why alternative approaches like ketamine have been studied.
Ketamine is a glutamate NMDA-receptor antagonist. Unlike SSRIs/SNRIs, which act on serotonin or norepinephrine, ketamine modulates glutamate, the primary excitatory neurotransmitter in the brain. This modulation appears to:
- Increase synaptic plasticity (brain flexibility)
- Rapidly improve mood within hours
- Potentially reduce suicidal thinking in some individuals
This mechanism is thought to “reset” dysfunctional neural circuits involved in mood regulation.
Ketamine is typically given as a subanesthetic intravenous (IV) infusion (commonly 0.5 mg/kg over ~40 minutes) and is administered alongside standard mood stabilizers to reduce risk of mood destabilization.
What the Research Says
Rapid Antidepressant Effects: Several controlled studies have found that a single IV ketamine infusion can significantly reduce depressive symptoms in people with treatment-resistant bipolar depression within 24–72 hours compared to placebo.
A systematic review pooling results from multiple studies (most using IV ketamine at 0.5 mg/kg) found:
- ~61 % response rate in bipolar depression participants after ketamine (≥50 % reduction in depressive severity)
- ~5 % response with placebo
- Improvements in symptoms like anhedonia and suicidal thinking
- Dissociation and transient blood pressure changes were the most common side effects reported.
Clinical Considerations
- Adjunctive Use: Ketamine is usually given with mood stabilizers (e.g., lithium, valproate) to reduce the risk of mood switching toward mania.
- Rapid Onset: Unlike traditional bipolar depression medications that can take weeks to work, ketamine may begin relieving symptoms within hours. This makes it of particular interest for acute depressive episodes where immediate improvement is critical.
- Duration of Effect: Ketamine’s antidepressant effects may be transient. Many patients require multiple sessions to maintain benefit, and research continues on optimal frequency and long-term protocols.
- Risk of Mood Elevation: Because bipolar disorder involves cycling between moods, clinicians monitor for mood instability, especially mania or hypomania. Most studies report this risk as low when ketamine is used with mood stabilizers, but it remains a considered safety factor.
Research Articles You Can Reference
Bahji et al. (2021) — Systematic Review on Ketamine for Bipolar Depression https://pubmed.ncbi.nlm.nih.gov/33929489/
Cochrane Review — Ketamine & Glutamate Modulators for Bipolar Depression https://www.cochrane.org/evidence/CD011611_ketamine-and-other-glutamate-receptor-modulat ors-bipolar-depression
Joseph et al. (2021) — Systematic Review on IV Ketamine in Bipolar Depression https://pubmed.ncbi.nlm.nih.gov/33347027/
Scoping Review — Ketamine in Treatment-Resistant Bipolar Depression. https://pubmed.ncbi.nlm.nih.gov/37371387/
NIMH Early Study on Rapid Ketamine Response in Bipolar Depression. https://www.nimh.nih.gov/news/science-updates/2010/experimental-medication-lifts-depressionsymptoms-in-bipolar-disorder-within-an-hour
Frontiers Article on Ketamine Mechanisms & Bipolar Depression. https://www.frontiersin.org/articles/10.3389/fpsyt.2022.867484/full
-
Ketamine Therapy for Trauma
Ketamine therapy is an emerging, scientifically studied option for adults experiencing symptoms from personal trauma, especially when standard treatments haven’t fully worked. It may reduce distressing symptoms quickly, enhance emotional processing, and support deeper healing when paired with psychotherapy. As with any medical treatment, ketamine should be administered under medical supervision and within a comprehensive care plan.
Many people with a history of personal trauma struggle with symptoms like intrusive memories, hypervigilance, anxiety, emotional numbing, and disrupted daily functioning. When symptoms persist, even after traditional therapy and medications, ketamine is one of the emerging treatment options being studied for its potential to help break patterns of trauma-related distress.
How Ketamine Works in Trauma-Related Conditions
Ketamine impacts the brain differently than traditional antidepressants. It blocks NMDA receptors (part of the glutamate system), which helps:
- Increase synaptic plasticity, making the brain more adaptable
- Modulate fear and memory circuits that are often overactive in trauma survivors
- Improve emotional processing and connectivity in key areas like the amygdala and hippocampus
- Reset dysfunctional fear responses and hyperreactivity that can underpin trauma symptoms
Ketamine & PTSD: What Research Says
Post-Traumatic Stress Disorder (PTSD) is one of the best-studied trauma-related conditions in ketamine research.
- Rapid Symptom Reduction: Randomized clinical trials show that a single intravenous ketamine infusion can meaningfully reduce core PTSD symptoms within 24 hours compared with an active control, with effects often noticeable even when depression is accounted for. https://jamanetwork.com/journals/jamapsychiatry/fullarticle/1860851
- Systematic Evidence of Benefit Meta-analyses of multiple studies conclude that ketamine is associated with significant improvements in PTSD symptom scales both shortly after treatment and after extended clinical courses. https://pmc.ncbi.nlm.nih.gov/articles/PMC10979792/
- Enhanced Trauma-Focused Therapy Emerging clinical research is exploring ketamine combined with trauma-focused therapies — for example, ketamine used alongside EMDR (Eye Movement Desensitization and Reprocessing). Early findings suggest symptom reductions and improved emotional processing that may go beyond ketamine alone. https://pubmed.ncbi.nlm.nih.gov/41186022
Durability with Repeated Treatment Open-label clinical trials pairing ketamine with structured trauma therapy (e.g., written exposure therapy) have shown large and lasting reductions in PTSD symptoms, sometimes lasting months after treatment completion. https://www.psychiatrist.com/jcp/combining-ketamine-infusions-and-written-exposure-therapy-chronic-ptsd-open-label-trial/
What This Means for Personal Trauma
Ketamine isn’t a “magic cure,” but research suggests it may help in several important ways for people dealing with trauma:
- Rapid relief of distressing symptoms: Many traditional treatments take weeks or months to work. Ketamine can reduce symptoms within hours in some cases.
- Increased emotional processing: By enhancing neuroplasticity, ketamine may help trauma survivors access and reframe traumatic memories in a therapeutic context.
- Synergy with psychotherapy: Ketamine may work best when combined with structured trauma-focused therapies such as EMDR or exposure-based approaches.
- Potential for longer-term improvement: Preliminary studies combining ketamine with ongoing therapy show symptom reductions that can persist for weeks or months.
Important Considerations
- Not for everyone: Ketamine can cause transient effects like dissociation, changes in perception, or emotional intensity, and experiences can vary widely. It should only be administered in a medical setting with monitoring.
- Trauma responses vary: Some people may find ketamine emotionally intense or triggering without structured therapeutic support. Research still has gaps, and individual responses can differ.
- Not a stand-alone: Ketamine is best seen as part of a comprehensive trauma care plan, ideally combined with trauma-informed psychotherapy and support.
Clinical Studies & Reviews
Intravenous Ketamine effective in chronic PTSD vs control: https://jamanetwork.com/journals/jamapsychiatry/article-abstract/1860851
Systematic review & meta-analysis showing PTSD symptom improvement: https://pmc.ncbi.nlm.nih.gov/articles/PMC10979792/
Ketamine + EMDR trauma processing study: https://pubmed.ncbi.nlm.nih.gov/41186022/ Open-label trial of ketamine combined with exposure therapy for PTSD: https://www.psychiatrist.com/jcp/combining-ketamine-infusions-and-written-exposure-therapy-ch ronic-ptsd-open-label-trial/
Mechanism & Neurobiology: Ketamine’s glutamate modulation and potential trauma mechanisms: https://www.sciencedirect.com/science/article/pii/S0197018621000905
Ketamine for pain
Ketamine is a medication originally developed as a surgical anesthetic. At sub-anesthetic doses, lower than what’s used for anesthesia, ketamine has been studied for pain relief because it blocks NMDA receptors, which are involved in pain transmission and central sensitization (chronic amplification of pain signals). It also appears to reduce opioid tolerance and inhibit pathways that contribute to persistent pain
-
Ketamine for cancer patients
How it might help
Cancer pain can be complex and multifactorial; from tumor-related nociception to neuropathic pain after treatment. Ketamine is sometimes used as an adjunct to opioids and standard analgesics in difficult-to-control cancer pain, particularly when pain is refractory to other approaches.
What the research shows
- A recent systematic review found that intravenous ketamine improved pain scores and reduced opioid use postoperatively in patients with cancer pain.
- Evidence for long-term chronic cancer pain relief is less consistent and appears to depend on dose, route, and patient population.
Azari et al. (2024): Systematic review of ketamine for acute and chronic cancer pain showing benefits mainly in the acute postoperative setting https://pubmed.ncbi.nlm.nih.gov/39201120/
-
Ketamine for Fibromyalgia
How it might help
Fibromyalgia involves central sensitization, where the nervous system becomes more sensitive to pain. Ketamine’s NMDA antagonism may reduce those sensitization effects.
What the research shows
- Clinical studies suggest short-term pain reduction after intravenous ketamine, typically only lasting a few hours after infusion.
- Some reports and case series suggest that higher or repeated doses may have longer effects, but strong long-term evidence is lacking.
Systematic review of IV ketamine for fibromyalgia shows short-term reductions in pain intensity. https://pubmed.ncbi.nlm.nih.gov/34984054/
-
Ketamine for Neuropathy
How it might help
Ketamine may reduce neuropathic pain by modulating central sensitization and the “wind-up” phenomenon at the spinal cord level.
What the research shows
- Systematic reviews and meta-analyses demonstrate that ketamine added to standard care can significantly lower neuropathic pain scores shortly after treatment and up to 30 days later.
- The evidence is stronger for short-term relief than for long-term sustained benefit. Pereira et al. (2022): Meta-analysis showing statistically significant reductions in neuropathic pain with ketamine. https://pubmed.ncbi.nlm.nih.gov/35431578/
-
Ketamine for Chronic Back Pain
How it might help
Chronic back pain often includes a neuropathic component and central sensitization. Ketamine’s NMDA blockade theoretically reduces pain signal amplification.
What the research shows
- Evidence is limited and mixed for chronic back pain specifically. Many clinical reviews describe weak to no clear evidence supporting routine use for chronic noncancer pain, including low-back pain.
- Ketamine may be considered in refractory cases when standard therapies have failed, but long-term data are lacking.
StatPearls review: Summarizes that ketamine has weak or no evidence for long-term relief in back pain outside of CRPS. https://www.statpearls.com/point-of-care/59718?utm_source=
-
Ketamine for Acute Injury Pain
How it might help
In acute pain (e.g., trauma or postoperative pain), ketamine can be used as part of a multimodal analgesia strategy, especially in emergency or surgical settings. It modulates pain pathways and can reduce opioid requirements.
What the research shows
- Umbrella reviews support beneficial effects of ketamine in acute pain management, particularly postoperatively or in emergency care.
- Ketamine may be particularly useful when opioids are insufficient or contraindicated.
MDPI umbrella review: Discussing ketamine’s role in acute pain management. https://www.mdpi.com/2077-0383/13/24/7699?utm_source=
-
Ketamine for Migraines
How it might help
Migraines involve abnormal neural excitability and central pain pathways. Some clinicians use ketamine particularly in refractory cases based on its NMDA antagonism and potential to interrupt pain signaling.
What the research shows
- Systematic reviews find mixed results overall, with some studies showing reduction in pain or aura severity and others showing no clear benefit compared to placebo or standard therapies.
- Some case series and retrospective analyses suggest short-term relief in refractory migraine.
- Overall evidence quality is low and more controlled trials are needed.
Chah et al. (2021): Systematic review of ketamine for migraine and other headaches showing mixed evidence. https://pubmed.ncbi.nlm.nih.gov/34703891/ Rangavijula et al. retrospective series: Suggests short-term benefit in refractory headaches. https://pharmaceutical-journal.com/article/news/ketamine-provides-short-term-relief-from-chronic-migraine?utm_source=
Ketamine for addiction management
Substance use disorders (addiction) whether to alcohol, cocaine, opioids, cannabis, or other drugs, involve powerful neural pathways that reinforce cravings, habitual use, and relapse. Traditional treatments (therapy, medications, behavioral support) help many people, but some individuals don’t respond fully or continue to struggle with cravings and relapse. That’s where research on ketamine as an adjunctive treatment is emerging. Ketamine is not a first-line or stand-alone treatment for addiction, but early research suggests it may help when integrated with therapy and support in a clinical setting. Research so far suggests it can reduce cravings, support abstinence, and help with withdrawal symptoms in conditions like alcohol, cocaine, opioids, and cannabis use disorders. However, evidence is still preliminary, and ketamine treatment should be considered within a comprehensive, medically supervised care plan.
How Ketamine Might Help in Addiction
-
Reducing Cravings and Use
Preliminary studies show that ketamine may:
- Decrease cravings for substances such as alcohol and cocaine.
- Increase abstinence rates or duration of abstinence when administered in controlled clinical settings, especially with supportive therapy.
For example, research suggests that ketamine infusion combined with psychotherapy can lead to:
- longer time to relapse
- fewer heavy drinking days
- greater likelihood of sustained abstinence in people with Alcohol Use Disorder (AUD).
-
Supporting Withdrawal Management
In alcohol withdrawal, ketamine has been studied as an adjunct to standard care and may:
- reduce severity of withdrawal symptoms
- decrease reliance on benzodiazepines in some difficult cases
However, more clinical trials are needed before definitive recommendations can be made.
-
Enhancing Therapy Engagement
Ketamine may temporarily increase neuroplasticity, the brain’s ability to reorganize and form new connections which can help people engage more deeply with psychotherapeutic interventions like motivational enhancement therapy or relapse prevention work.
This potential “window of enhanced learning” is an active area of research, and combining ketamine with structured therapy appears to yield better outcomes than ketamine alone in many studies.
Alcohol Use Disorder (AUD)
- Ketamine has been linked with:
- reduced alcohol consumption
- increased abstinence duration
- reduced cravings, particularly when combined with psychotherapy.
- Some studies report earlier resolution of severe withdrawal symptoms (e.g., delirium tremens) when ketamine is used as an adjunct with standard treatment, though more research is needed.
- Articles:
- Ketamine Treatment for Alcohol Use Disorder: A Systematic Review — Ketamine may help reduce alcohol use and cravings. https://pubmed.ncbi.nlm.nih.gov/37273364/
- Scoping Review: Ketamine in AUD and Withdrawal — promising but requires more evidence. https://pubmed.ncbi.nlm.nih.gov/37181899/
- Review in European Psychiatry: Ketamine + therapy may prolong abstinence. https://www.cambridge.org/core/journals/european-psychiatry/article/keta mine-treatment-for-alcohol-use-disorder-a-review/5D3403855E6D45C36 CD8318FEABB95C9?utm_source=
Opioid Use Disorder (OUD)
- Some small studies included in recent reviews show increased abstinence and reduced craving when ketamine is used within therapeutic protocols.
- Evidence is still limited by sample size and study design.
- Articles:
- Systematic review: Ketamine shows potential benefits across SUDs including opioids. https://pubmed.ncbi.nlm.nih.gov/40320049/
Cannabis Use Disorder (CNUD)
- Very limited data, but early results indicate ketamine may help reduce weekly cannabis use and increase confidence in abstinence in some participants.
- Articles:
- Ketamine’s effects in cannabis use disorder. https://pubmed.ncbi.nlm.nih.gov/40320049
Important Safety & Clinical Considerations
-
Not a Stand-Alone Treatment
Ketamine is not a replacement for evidence-based addiction treatments (like counseling, medication-assisted therapy, or support programs). It may be used as an adjunct under medical supervision.
-
Risk of Misuse & Monitoring
Ketamine itself has misuse potential outside a clinical setting, especially at higher, unsupervised doses and should be given by a medical provider in a setting with monitoring.
Therapeutic programs typically include psychotherapy and integration sessions to help translate insights into long-term behavior change.
Ketamine for addiction management
Substance use disorders (addiction) whether to alcohol, cocaine, opioids, cannabis, or other drugs, involve powerful neural pathways that reinforce cravings, habitual use, and relapse. Traditional treatments (therapy, medications, behavioral support) help many people, but some individuals don’t respond fully or continue to struggle with cravings and relapse. That’s where research on ketamine as an adjunctive treatment is emerging. Ketamine is not a first-line or stand-alone treatment for addiction, but early research suggests it may help when integrated with therapy and support in a clinical setting. Research so far suggests it can reduce cravings, support abstinence, and help with withdrawal symptoms in conditions like alcohol, cocaine, opioids, and cannabis use disorders. However, evidence is still preliminary, and ketamine treatment should be considered within a comprehensive, medically supervised care plan.
How Ketamine Might Help in Addiction
-
Reducing Cravings and Use
Preliminary studies show that ketamine may:
- Decrease cravings for substances such as alcohol and cocaine.
- Increase abstinence rates or duration of abstinence when administered in controlled clinical settings, especially with supportive therapy.
For example, research suggests that ketamine infusion combined with psychotherapy can lead to:
- longer time to relapse
- fewer heavy drinking days
- greater likelihood of sustained abstinence in people with Alcohol Use Disorder (AUD).
-
Supporting Withdrawal Management
In alcohol withdrawal, ketamine has been studied as an adjunct to standard care and may:
- reduce severity of withdrawal symptoms
- decrease reliance on benzodiazepines in some difficult cases
However, more clinical trials are needed before definitive recommendations can be made.
-
Enhancing Therapy Engagement
Ketamine may temporarily increase neuroplasticity, the brain’s ability to reorganize and form new connections which can help people engage more deeply with psychotherapeutic interventions like motivational enhancement therapy or relapse prevention work.
This potential “window of enhanced learning” is an active area of research, and combining ketamine with structured therapy appears to yield better outcomes than ketamine alone in many studies.
Alcohol Use Disorder (AUD)
- Ketamine has been linked with:
- reduced alcohol consumption
- increased abstinence duration
- reduced cravings, particularly when combined with psychotherapy.
- Some studies report earlier resolution of severe withdrawal symptoms (e.g., delirium tremens) when ketamine is used as an adjunct with standard treatment, though more research is needed.
- Articles:
- Ketamine Treatment for Alcohol Use Disorder: A Systematic Review — Ketamine may help reduce alcohol use and cravings. https://pubmed.ncbi.nlm.nih.gov/37273364/
- Scoping Review: Ketamine in AUD and Withdrawal — promising but requires more evidence. https://pubmed.ncbi.nlm.nih.gov/37181899/
- Review in European Psychiatry: Ketamine + therapy may prolong abstinence. https://www.cambridge.org/core/journals/european-psychiatry/article/keta mine-treatment-for-alcohol-use-disorder-a-review/5D3403855E6D45C36 CD8318FEABB95C9?utm_source=
Opioid Use Disorder (OUD)
- Some small studies included in recent reviews show increased abstinence and reduced craving when ketamine is used within therapeutic protocols.
- Evidence is still limited by sample size and study design.
- Articles:
- Systematic review: Ketamine shows potential benefits across SUDs including opioids. https://pubmed.ncbi.nlm.nih.gov/40320049/
Cannabis Use Disorder (CNUD)
- Very limited data, but early results indicate ketamine may help reduce weekly cannabis use and increase confidence in abstinence in some participants.
- Articles:
- Ketamine’s effects in cannabis use disorder. https://pubmed.ncbi.nlm.nih.gov/40320049
Important Safety & Clinical Considerations
-
Not a Stand-Alone Treatment
Ketamine is not a replacement for evidence-based addiction treatments (like counseling, medication-assisted therapy, or support programs). It may be used as an adjunct under medical supervision.
-
Risk of Misuse & Monitoring
Ketamine itself has misuse potential outside a clinical setting, especially at higher, unsupervised doses and should be given by a medical provider in a setting with monitoring.
Therapeutic programs typically include psychotherapy and integration sessions to help translate insights into long-term behavior change.
About Ketamine Therapy
A Well-Established Medication with Evolving Uses

Ketamine has been used in medicine for decades and was approved by the FDA in 1970 for anesthesia and pain control. It remains on the World Health Organization’s List of Essential Medicines. Today, in low-dose, medically monitored settings, ketamine is explored as a supportive tool for individuals experiencing certain mental health symptoms or chronic pain. Research suggests it may promote neuroplasticity, helping people feel less “stuck” in long-standing emotional or physical patterns.
A Guided Addition to Your Wellness Plan
Modern studies continue to examine how ketamine may influence brain networks involved in distressing or repetitive thought cycles. Because of these emerging insights, ketamine is used off-label as an adjunctive option—not a cure and not a replacement for comprehensive care. At Prime Youth Aesthetics, ketamine infusions are administered intravenously in a structured, medically supervised setting designed to support individuals navigating persistent mood-related challenges or chronic pain symptoms with safety, clarity, and compassion.
How It Works
What does Ketamine do to your brain?
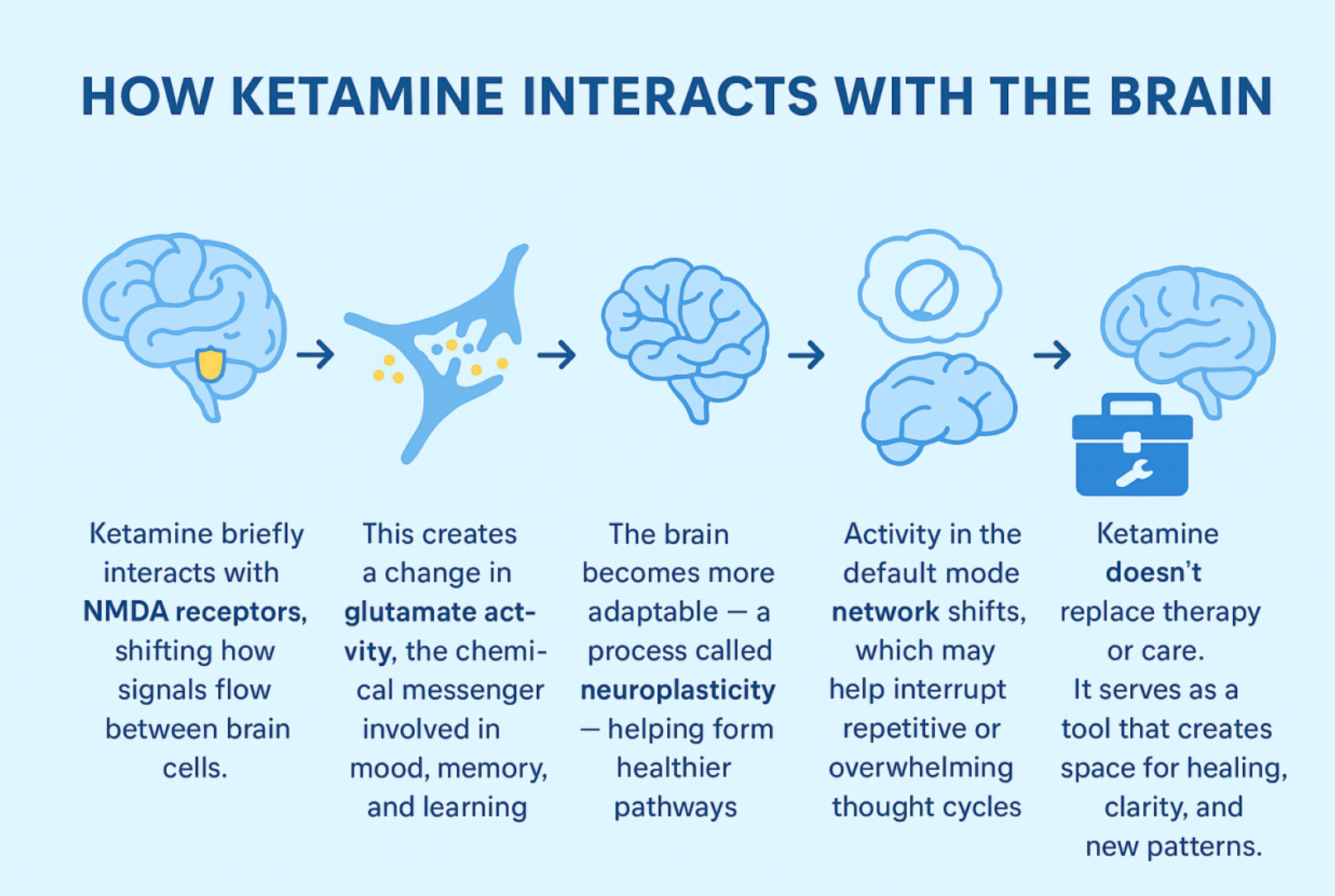
Ketamine interacts with a system in the brain called the NMDA receptor, which plays a role in how your brain cells communicate. By briefly blocking this receptor, ketamine creates a shift in how the brain uses glutamate, a chemical that helps with learning, memory, and emotional processing. This shift can encourage the brain to become more flexible, making it easier to form healthier patterns, break out of unhelpful thought cycles, and respond differently to stress.
Ketamine also interacts with regions involved in pain modulation. Some studies show changes in activity in the anterior cingulate cortex, insula, and thalamus, areas tied to the perception and emotional response to pain. These interactions are part of why ketamine is being explored as a supportive tool for certain chronic pain conditions.
Overall, ketamine acts as a tool that helps create a window of opportunity for emotional healing, new habits, or supportive therapies to work more effectively.
A Guided Addition to Your Wellness Plan

Modern studies continue to examine how ketamine may influence brain networks involved in distressing or repetitive thought cycles. Because of these emerging insights, ketamine is used off-label as an adjunctive option—not a cure and not a replacement for comprehensive care. At Prime Youth Aesthetics, ketamine infusions are administered intravenously in a structured, medically supervised setting designed to support individuals navigating persistent mood-related challenges or chronic pain symptoms with safety, clarity, and compassion.
How It Works
What does Ketamine do to your brain?
Ketamine interacts with a system in the brain called the NMDA receptor, which plays a role in how your brain cells communicate. By briefly blocking this receptor, ketamine creates a shift in how the brain uses glutamate, a chemical that helps with learning, memory, and emotional processing. This shift can encourage the brain to become more flexible, making it easier to form healthier patterns, break out of unhelpful thought cycles, and respond differently to stress.
Ketamine interacts with a system in the brain called the NMDA receptor, which plays a role in how your brain cells communicate. By briefly blocking this receptor, ketamine creates a shift in how the brain uses glutamate, a chemical that helps with learning, memory, and emotional processing. This shift can encourage the brain to become more flexible, making it easier to form healthier patterns, break out of unhelpful thought cycles, and respond differently to stress.
Overall, ketamine acts as a tool that helps create a window of opportunity for emotional healing, new habits, or supportive therapies to work more effectively.
Contact Us Today
Reach out to us if you want to know more, have any questions, concerns, or to schedule a consultation or service— we're here to assist you on your journey to renewed beauty!

